Food allergies don’t always make themselves known right away. While some reactions strike within minutes — a swollen lip, a sudden rash, or a tightening throat — others take hours or even days to surface. These slower, harder-to-trace reactions are called delayed food allergies, and because they don’t follow the dramatic, obvious pattern most people associate with allergies, they’re frequently misunderstood, missed entirely, or blamed on something else.
According to FARE (Food Allergy Research & Education), food allergies affect millions of people worldwide — yet delayed-type reactions, driven by IgG antibodies rather than IgE, remain significantly underdiagnosed. If you’ve ever felt sluggish, bloated, or broken out in a rash the day after a meal and couldn’t figure out why, a delayed food allergy may be the underlying cause.
What Is a Delayed Food Allergy?
A delayed food allergy — sometimes called a late-onset food allergy, IgG food intolerance, or food sensitivity — is an immune response that occurs when the body produces antibodies against specific proteins found in certain foods or drinks. Unlike classic immediate allergic reactions, where the immune system responds within minutes via IgE antibodies, delayed food allergies are driven by IgG antibodies — a different arm of the immune system that reacts much more slowly.
The result is inflammation, discomfort, and a range of delayed food allergy symptoms that can affect almost any system in the body. Symptoms may begin anywhere from two hours to three full days after eating the triggering food — making it genuinely difficult to connect what you ate on Tuesday with how you’re feeling on Thursday. According to the NIH MedlinePlus immunoglobulin reference, elevated IgG levels against specific food proteins are a measurable marker of this type of delayed sensitivity.
How Delayed Allergies Differ from Immediate Allergies
Understanding this distinction matters not just for diagnosis, but for treatment. Someone managing a delayed food allergy doesn’t need an EpiPen — they need to identify and eliminate the foods quietly triggering their immune system. Here’s how the two types compare:
| Feature | Immediate Allergy | Delayed Food Allergy (IgG) |
| Onset time | Minutes | 2 hours to 3 days |
| Antibody type | IgE | IgG |
| Typical severity | Often severe / anaphylactic | Mild to moderate |
| Ease of diagnosis | Relatively clear trigger | Much harder to trace |
| Common treatment | Epinephrine, antihistamines | Elimination diet, dietary change |
Why Delayed Food Allergies Are Often Overlooked
There are several reasons delayed food allergies — including what doctors sometimes classify as IgG food sensitivity — go undetected for years, even decades:
- The dose matters. Eating a small amount of the triggering food may produce no noticeable symptoms. Reactions are more likely after consuming a larger portion, or after eating the same food repeatedly across several days.
- Favourite foods are common culprits. Because reactions don’t happen immediately, people never suspect foods they eat regularly. The foods consumed most often are statistically the most likely to be causing low-grade chronic reactions.
- Symptoms are non-specific. Fatigue, bloating, headaches, and skin issues — all classic delayed food sensitivity symptoms — can have dozens of causes. Without a clear link to a specific meal, food is rarely considered the trigger.
- Any organ can be affected. Unlike immediate allergies that typically hit the skin or airways, delayed food allergies can manifest in virtually any tissue — joints, sinuses, the brain, the digestive tract — making them easy to confuse with other conditions.
Common Symptoms of Delayed Food Allergies
Because delayed reactions can affect so many different systems, the symptom list is broad. The most frequently reported delayed food allergy symptoms include:
- Bloating, gas, cramping, or diarrhoea — often the first sign of a food allergy-related digestive reaction
- Persistent skin rashes, eczema and allergen-driven skin flare-ups, or unexplained itching
- Chronic fatigue or low energy, particularly after meals
- Brain fog, difficulty concentrating, or mental sluggishness
- Recurring headaches or migraines
- Joint pain, stiffness, or inflammation — a less widely known but documented delayed reaction
- Nasal congestion, postnasal drip, or sinus pressure
- Mood fluctuations, irritability, or anxiety
- Sleep disturbances with no clear cause
None of these symptoms alone proves a delayed food allergy — but a consistent pattern of feeling unwell hours or days after eating, with no other explanation, is a strong indicator worth investigating.
How Delayed Food Allergy Testing Works
If you suspect a delayed food allergy or IgG food sensitivity, a physician or allergist can recommend one or more diagnostic approaches for food allergy testing. The American College of Allergy, Asthma & Immunology (ACAAI) recommends working with a board-certified allergist to determine the most appropriate test for your situation.
Skin Prick Testing
In a skin prick test, small amounts of known allergens are applied to the skin surface. The test site is monitored for swelling, redness, or itching — reactions that typically appear within 15–20 minutes. The larger the skin reaction, the greater the sensitivity to that allergen. Side effects — localized redness or swelling — resolve within one to two days. If symptoms persist beyond 48 hours, contact your doctor.
IgG Blood Test (Food Allergy Panel)
Blood testing is particularly valuable for identifying delayed reactions. The most common method — the IgG blood test for food allergy — measures the concentration of immunoglobulins released when the body encounters specific foods. Elevated IgG levels against a particular food protein are a marker of delayed sensitivity. A standard IgG food panel can screen reactions to dozens or even hundreds of foods in a single blood draw, providing a comprehensive picture of hidden sensitivities. For those wondering about the best IgG food sensitivity test options, panels vary from 50 to 450+ foods depending on the laboratory.
Food Intolerance Blood Test (ELISA)
The enzyme-linked immunosorbent assay — ELISA — is a highly sensitive food intolerance blood test that uses antibody-antigen interactions to detect immune responses to specific food proteins. According to published NIH methodology, standard ELISA food panels can screen up to 95 foods simultaneously, making them one of the most comprehensive tools available. For broader screening, allergy food sensitivity panels and MRT food sensitivity testing measure cellular reactions across 450+ foods.
The Elimination Diet
When laboratory tests are inconclusive, or when a patient wants to confirm results through lived experience, the elimination diet protocol recommended by Mayo Clinic is often the gold standard. This involves removing all suspected trigger foods for 4–6 weeks, then reintroducing them one at a time while carefully monitoring for symptom recurrence. Though it requires patience and food journaling, it remains one of the most definitive ways to identify delayed food sensitivity symptoms — because it relies on the body’s own response rather than indirect lab markers.
Foods That Commonly Trigger Delayed Allergic Reactions
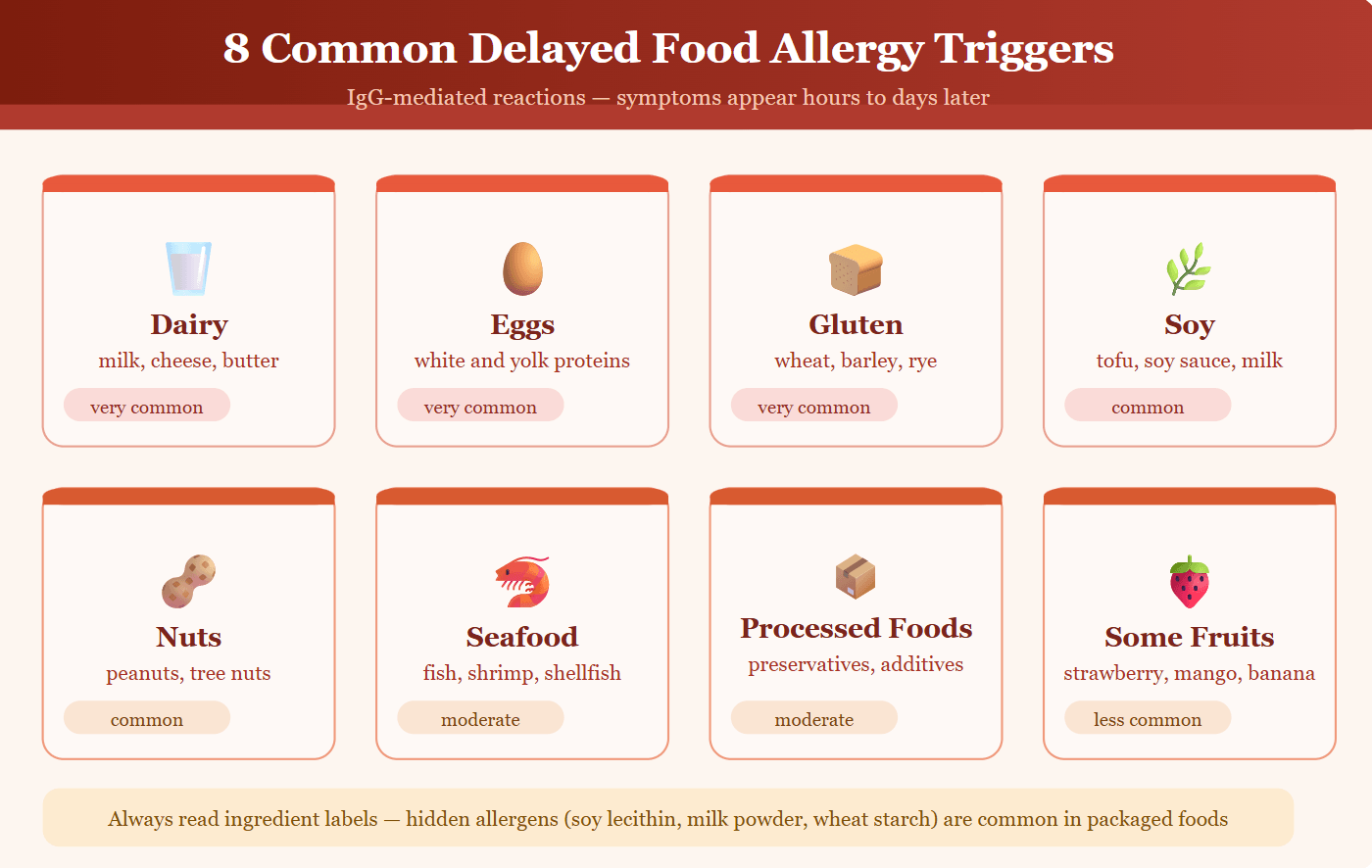
While any food can theoretically cause a delayed reaction in a sensitive individual, certain foods are responsible for the vast majority of cases. These are the most frequently reported triggers:
- Dairy products — particularly cow’s milk, which is highly concentrated in proteins that some immune systems cannot tolerate. A delayed reaction to dairy is one of the most common delayed-type food sensitivities in adults.
- Eggs — a high-protein food that triggers delayed reactions in both children and adults, typically presenting as skin rashes or digestive discomfort rather than immediate anaphylaxis.
- Gluten intolerance vs gluten allergy — wheat, barley, and rye all contain gluten, which triggers both celiac disease and non-celiac sensitivity. Many processed foods contain hidden gluten sources not obvious from the label.
- Soy and soy-derived products — soybeans, tofu, soy sauce, and soy milk frequently trigger delayed sensitivities, especially in early childhood.
- Peanuts and tree nuts — among the most protein-dense foods, nuts can cause both immediate and delayed reactions. Read labels carefully for cross-contamination warnings.
- Seafood — fish, shrimp, crab, and shellfish contain proteins the immune system of a sensitive person treats as hostile. Reactions can develop even from small amounts.
- Processed foods with preservatives — artificial colourings, preservatives, and flavour enhancers can trigger or amplify immune responses in sensitive individuals.
- Certain fruits and vegetables — strawberries, mango, banana, watermelon, and spinach are among the more commonly reported plant-based triggers, particularly in children.
⚠️ Always read ingredient labels carefully. Many packaged foods contain hidden allergens — soy lecithin, milk powder, wheat starch — that aren’t immediately obvious from the product name.
Foods That Support the Body During Allergic Reactions
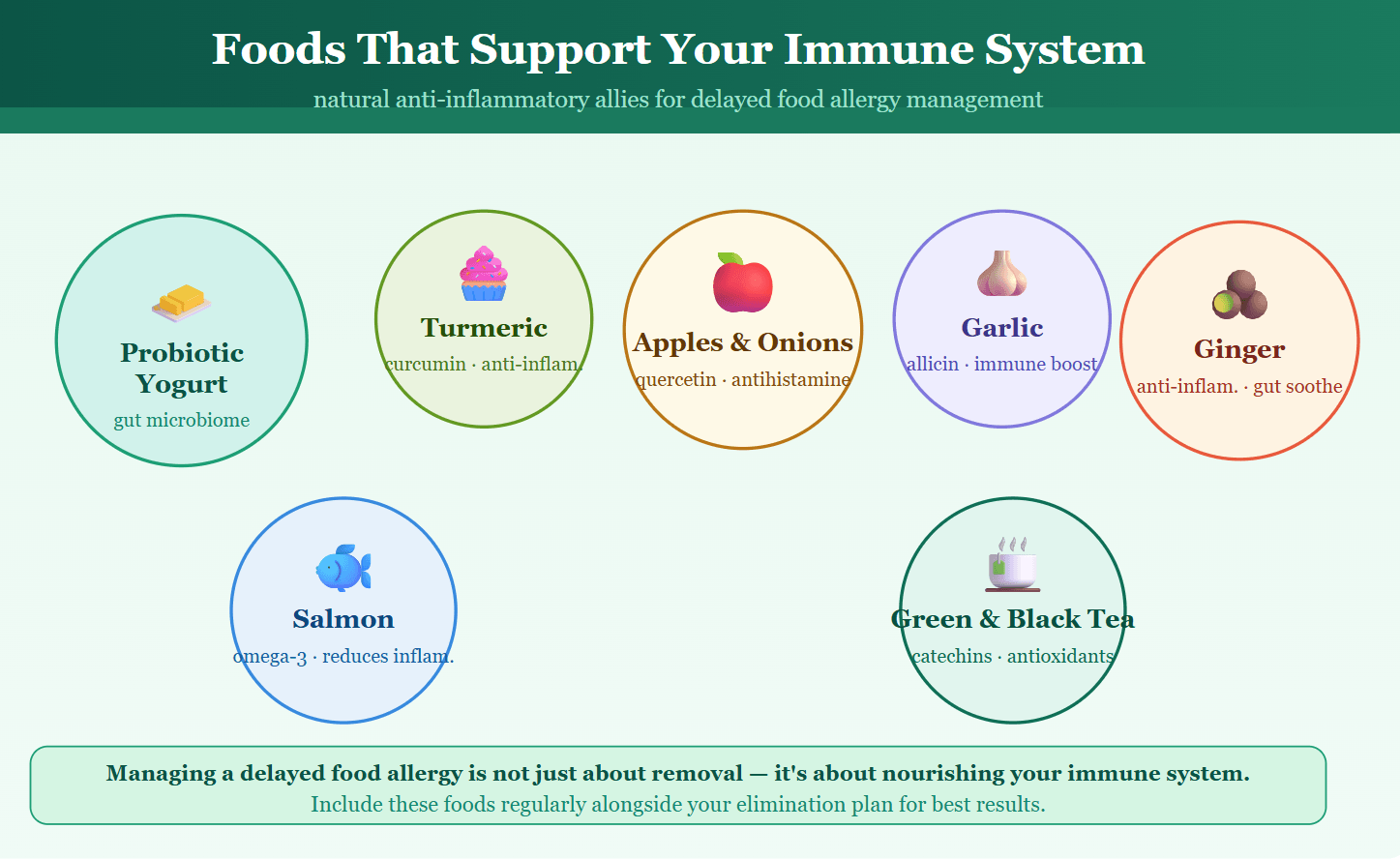
Managing a delayed food allergy isn’t solely about removing foods — it’s also about nourishing the immune system. Research on quercetin as a natural antihistamine and other compounds found in everyday foods shows measurable benefits in reducing allergic inflammation. Here are the top foods to incorporate:
| Food | Why It Helps |
| Probiotic yogurt | Supports gut microbiome balance — a healthy gut is the foundation of a well-regulated immune response. |
| Turmeric | Contains curcumin, a potent natural anti-inflammatory. Reduces histamine activity and inflammatory markers. |
| Apples & onions | Rich in quercetin, a natural flavonoid with antihistamine and mast-cell-stabilising properties. |
| Garlic | Organosulfur compounds (allicin) provide antimicrobial and immune-boosting effects — one of the most studied foods for immune support. |
| Ginger | Natural anti-inflammatory and digestive soother. Helps calm gut irritation triggered by delayed food reactions. |
| Salmon & mackerel | High in omega-3 fatty acids, which actively reduce systemic inflammation and balance the immune response. |
| Green & black tea | Catechins and antioxidants support immune regulation, reducing allergy frequency over time. |
When to See a Doctor
Delayed food allergies rarely cause the dramatic reactions associated with immediate allergies — but they can significantly reduce quality of life over time, and in some cases worsen into more serious conditions if left unmanaged.
Seek medical advice if you notice:
- Recurring digestive problems — bloating, cramping, or diarrhoea — with no identifiable cause
- Chronic skin conditions like eczema, rashes, or hives
- Persistent fatigue or brain fog that follows meals
- Joint pain or inflammation with no injury or arthritis diagnosis
- Any symptom that seems to follow a meal pattern, even loosely
A board-certified allergist or immunologist can guide you through appropriate testing and develop a personalised management plan — which may include dietary adjustments, antihistamine support, gut-healing protocols, or allergy desensitisation / immunotherapy to reduce long-term sensitivity. You can find a board-certified allergist near you via ACAAI.
✅ Early diagnosis and a structured response make an enormous difference. Delayed food allergies are manageable — but only once they’re identified.

